Once infected with a herpes virus, it lies dormant in the body, waiting for the next chance. Researchers have now discovered how the virus reactivates itself. This could also be important for Long-COVID research.
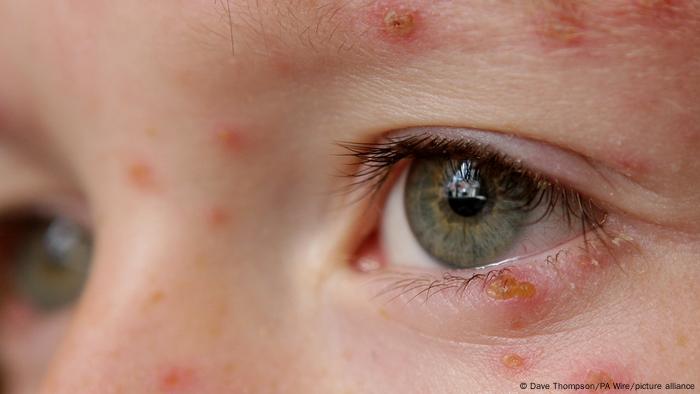
The first infection with a herpes virus can be unpleasant. Permanent reactivation causes real problems.
Chickenpox is a vivid example. The cause of the itchy skin blisters is one of the nine known herpes viruses that can infect and make people ill, the varicella-zoster virus. It is widespread worldwide and is best known as a childhood disease. Most of the time, the little ones put the infection away well, a few scars may remain from scratching. And the virus stays, too.
The varicella-zoster variant of the herpes virus settles in the nerve cell bodies, the so-called ganglia. It can reawaken years or decades later and come back in the form of shingles.
In addition to the varicella zoster virus, the herpes virus family also includes the herpes simplex viruses type 1 and 2. They are known worldwide because they are responsible for painful cold sores and genital herpes. The cytomegalovirus is also widespread and can lead to severe complications and organ damage, especially in immunosuppressed people.
Epstein-Barr virus and Kaposi's sarcoma-associated herpesvirus can cause tumors. The human herpesviruses 6 (often divided into A and B) and 7 are also widespread and trigger, for example, the three-day fever known as a childhood disease.
Watch video 09:09
Herpes and shingles – sick with viruses
“The most important thing about herpes viruses is that they remain latent in the body for a lifetime after the primary infection,” says Lars Dölken, virologist at the University of Würzburg. Dölken thus names the most important thing this virus family has in common ;understand together with research colleagues which mechanism is behind the sudden awakening of the pathogens and has therefore examined the human herpesvirus 6A (HHV-6A) under the magnifying glass. The research team published the result in a study in the journal Nature: they discovered nothing less than a previously unknown cellular mechanism that the virus uses to wake up from sleep.
Between sleeping and waking
Anyone who catches a herpes virus for the first time often does not even notice it. The problems are usually caused by the repeated reactivation of the virus. To do this, it often uses a phase in which the host's immune system is already fighting on other fronts. This can be a cold, as well as severe physical and mental stress. People with HIV or transplant patients are particularly susceptible.
HHV-6A builds itself into the genome of the human cell and survives there in the latency phase until there is a good opportunity for the virus to attack again and thus multiply. Then a specific micro-RNA goes to work and reactivates the virus.
“Almost all herpesviruses produce their own micro-RNAs, which are extremely important for the virus. But there is no example of a herpes virus, where the micro-RNA is so fundamental,” says the virologist Dölken. “If we switch off this one viral micro-RNA, then the virus is – to put it a bit imprecisely – dead.”
A viral micro-RNA as master regulator
Unlike mRNA, for example, microRNA is not responsible for carrying the blueprint for certain proteins – it belongs to the non-coding RNAs. Instead, the viral micro-RNA interferes with the metabolism of certain human micro-RNAs and inhibits their development.
As a result, the production of so-called type I interferons is disrupted. These are messenger substances with which the cell reports the presence of viruses to the immune system. “But that is certainly not the only mechanism that is disrupted,” says Dölken. The researchers only scratched the surface with their investigation.
The viral micro-RNA makes it possible for the herpes viruses to evade the immune system, or to be more precise, the B and T cells that infect human cells eliminate. “These cells recognize foreign proteins – for example those of a virus.
“However, with the help of RNA, the herpes viruses manage to reprogram the host cells and use them to their advantage without our learned immune system, i.e. B and T cells, having a chance of recognizing the cell as infected,” explains Dölken.
Watch video 26:01
COVID-19 special: Long-COVID – symptoms and therapies
From COVID-19 to herpes to Long-COVID?
The The discovery of the one crucial viral micro-RNA, the “master regulator” as Dölken calls it, not only made it possible for the researchers in the cell culture experiment to prevent the reactivation of the herpes virus.
Conversely, the findings and further research could also help in the future to reactivate latent cells in the body, which the immune system can then recognize and render harmless. “Before transplanting an organ, it would be good to be able to switch off cells latently infected with herpes virus,” says Dölken.
With their research, the Würzburg virologists could also contribute to solving another problem: Long-COVID. Since herpesviruses often attack an already weakened immune system, scientists also suspect them of being involved in the various clinical pictures of long-COVID. “One obvious assumption is that herpes viruses are reactivated due to the corona infection and secondary damage occurs as a result,” says Dölken. There are still more questions than answers. But at least there are a few prime suspects. HHV-6 is one of them.
 Viruses and bacteria don't stand a chance – with a strong immune system
Viruses and bacteria don't stand a chance – with a strong immune system Viruses and bacteria don't stand a chance – with a strong immune system
Viruses and bacteria don't stand a chance – with a strong immune system Viruses and bacteria don't stand a chance – with a strong immune system
Viruses and bacteria don't stand a chance – with a strong immune system Viruses and bacteria don't stand a chance – with a strong immune system
Viruses and bacteria don't stand a chance – with a strong immune system Viruses and bacteria don't stand a chance – with a strong immune system
Viruses and bacteria don't stand a chance – with a strong immune system Viruses and bacteria don't stand a chance – with a strong immune system
Viruses and bacteria don't stand a chance – with a strong immune system Viruses and bacteria don't stand a chance – with a strong immune system
Viruses and bacteria don't stand a chance – with a strong immune system Viruses and bacteria don't stand a chance – with a strong immune system
Viruses and bacteria don't stand a chance – with a strong immune system No chance for Viruses and bacteria – with a strong immune system
No chance for Viruses and bacteria – with a strong immune system